Breathwork for Trauma Healing
Breathwork for Trauma Healing: A Beginner’s Guide to Nervous System Recovery
The practice of conscious breathing — commonly known as breathwork — sits at a remarkable crossroads between ancient somatic wisdom and modern neuroscience. When it comes to trauma recovery, breathwork can be understood as a purposeful shift in breathing patterns that may influence your physical, mental, and emotional state. For beginners making sense of the complexities of trauma, breathwork offers a unique doorway into the autonomic nervous system – a way to gently regulate physiological arousal that is often out of reach through traditional talk therapy alone.
This guide walks through the foundational mechanisms of breathwork, its grounding in Polyvagal Theory, the growing body of clinical evidence supporting its use, and the somatic frameworks you’ll need to practise it safely.
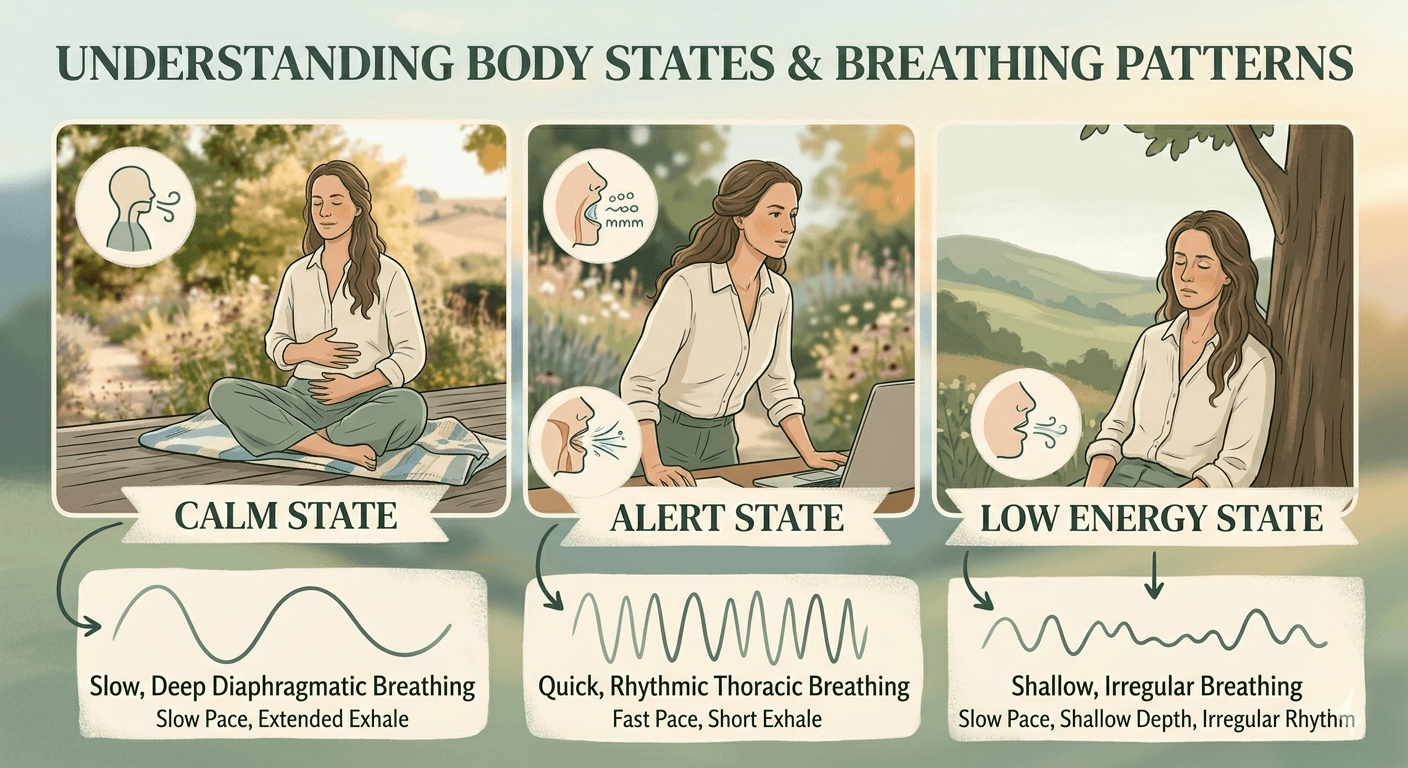
Autonomic Nervous System States
Physiological markers, breathing patterns & associated trauma responses
| Autonomic State | Physiological Markers | Impact on Breathing | Associated Trauma Response |
|---|---|---|---|
| Ventral Vagal | Regulated heart rate, social connectivity | Slow, deep, diaphragmatic | Safety and connection |
| Sympathetic | Increased cortisol, high alertness | Rapid, shallow, upper-chest | Fight or Flight |
| Dorsal Vagal | Persistent fatigue, emotional numbness | Shallow, restricted, or breath-holding | Freeze or Shutdown |
Breathwork vs Meditation: Which Is Right for Trauma?
A common question beginners ask is how breathwork differs from traditional meditation. While both practices aim to improve well-being, they work through fundamentally different mechanisms. Meditation is generally a passive practice of observation — it encourages you to notice thoughts and sensations without judgement. For many trauma survivors, however, the stillness that meditation requires can be counterproductive: the quiet can lead to dissociation, or allow traumatic memories to surface in an overwhelming way.
Breathwork is an active intervention. It gives the nervous system a clear, physical task — and that tangibility makes it a far more accessible starting point for those whose systems are highly activated. By giving an “activated system something to do,” breathwork can act as a bridge, gently bringing the stress response down until a calmer, more settled state is reached. This “bottom-up” approach — changing the body to shift the mind — is often more immediately effective for acute stress than the “top-down” work of cognitive mindfulness. If you already practise gentle, body-based movement and mindfulness, breathwork makes a natural companion practice that extends the same principles into the breath.
Breathwork vs. Meditation
A comparative look at two powerful mind-body practices
| Feature | Breathwork | Meditation |
|---|---|---|
| Method | Active control and intervention | Passive observation and awareness |
| Primary Goal | Immediate state change and regulation | Long-term awareness and resilience |
| Learning Curve | Generally shorter and more intuitive | Requires more practice and discipline Steeper |
| Somatic Impact | Direct influence on HRV and cortisol | Changes in brain structure (grey matter) |
| Application | Emergency "reset" button Immediate | Long-term "navigation system" Sustained |
What the Research Says — Breathwork for PTSD and Anxiety
Breathwork has moved steadily from the edges of wellness into clinically validated territory, supported by a growing body of peer-reviewed research. Structured breathing protocols have been shown in clinical trials to produce meaningful improvements in symptoms of Post-Traumatic Stress Disorder (PTSD), generalised anxiety, and depression.
The A52 Breath Method and Paramedicine Resilience
One notable study — a single-blind randomised controlled trial published on PubMed Central (NIH) — focused on paramedicine students, a group with disproportionately high rates of PTSD and anxiety. The A52 Breath Method involves a 5-second nasal inhalation, a 5-second exhalation, and a 2-second post-exhalatory hold, repeated over ten minutes.
Participants in the breathwork group reported significantly lower stress and anxiety scores, as well as higher resilience, compared to control groups. In their own words, students described the practice as a “coping tool” that gave them a sense of psychological safety and control during high-pressure clinical placements.
Sudarshan Kriya Yoga (SKY) in Veteran Populations
Sudarshan Kriya Yoga (SKY) — a sequence of breathing exercises that moves through varying breathing rates — has shown real promise for veterans living with clinically significant PTSD symptoms. Research suggests it may be as effective as traditional Cognitive Processing Therapy (CPT) in reducing PTSD symptom severity, with this work documented in a registered clinical trial via ClinicalTrials.gov. The physiological benefits may include improved Heart Rate Variability (HRV) — a key marker of autonomic balance and the body’s capacity to recover from stress.
A Wide-Ranging Meta-Analysis of Breathwork for Mental Health
A wide-ranging 2023 meta-analysis of 12 randomised controlled trials — involving 785 adults — found that breathwork interventions were significantly associated with lower levels of subjective stress. The review highlighted a strong safety profile for slow-paced breathing techniques, though it urged particular caution around fast-paced techniques with vulnerable or clinical populations until further research is available. The evidence points to human-guided training, sessions of at least five minutes, and consistent long-term practice as the most effective approach.
Breathwork Interventions: Clinical Evidence
Selected studies on controlled breathing techniques for stress, anxiety, and nervous system regulation
| Study / Protocol | Population | Key Findings | Metric Improved |
|---|---|---|---|
| A52 Method (PMC RCT)
Randomized Controlled Trial
|
Paramedicine students | Lower anxiety and depression | Resilience scores |
| SKY Breath
Sudarshan Kriya Yoga
|
Veterans with PTSD | Normalised anxiety levels | HRV and Sleep |
| 2023 Meta-Analysis
Systematic Review
|
General adults | Significant reduction in stress | Self-reported stress |
| Slow Breathing Interventions
Clinical Review
|
Anxiety patients | Targeting dysfunctional patterns | Parasympathetic activation |
Somatic Principles for Trauma-Informed Breathwork
For beginners, the power of breathwork needs to be matched with a genuine commitment to safety. The idea that “more is better” can be genuinely harmful in trauma recovery — intense breathing patterns have the potential to trigger emotional flooding or re-traumatisation. If you are already working to manage pain and fatigue flare-ups holistically, the same principle applies here: slow, titrated approaches are always safer than intensity. Practitioners draw on three core principles from Somatic Experiencing to guard against overwhelm: Resourcing, Titration, and Pendulation.
Resourcing — Establishing Internal Safety
Resourcing is the practice of identifying and connecting with internal or external anchors that bring a sense of safety and groundedness. For many trauma survivors, the body can feel like an unsafe place to be. Resourcing works to expand the “Window of Tolerance” — the optimal zone of arousal where healing is possible — by helping the nervous system remember that it can access calm states. In a breathwork session, a resource might be as simple as noticing the sensation of your back against a chair, a calming visualisation, or a neutral body part such as the big toe or earlobe.
Titration — Processing in Small Steps
Titration is the practice of slowing down and approaching trauma in small, manageable steps. Because trauma is often described as “too much, too fast, too soon,” titration works in the opposite direction — touching only small “bits” of a difficult experience at a time. In practice, this might mean breathing into a single small area of tension rather than the whole body, or bringing gentle awareness to a mildly uncomfortable memory rather than the full weight of a traumatic event. This approach means the nervous system is not overwhelmed and can begin to integrate what arises.
Pendulation — The Rhythm of Integration
Pendulation describes the natural oscillation between states of contraction (activation, trauma) and expansion (resourced safety). A resilient nervous system is one that can move fluidly between these states without becoming stuck. In trauma-informed breathwork, a facilitator guides you to pendulate between the intensity of a somatic release and the comfort of a resource. Over time, this process may help rewire the relationship between activation and safety – showing the nervous system that even intense moments can be followed by a return to calm.
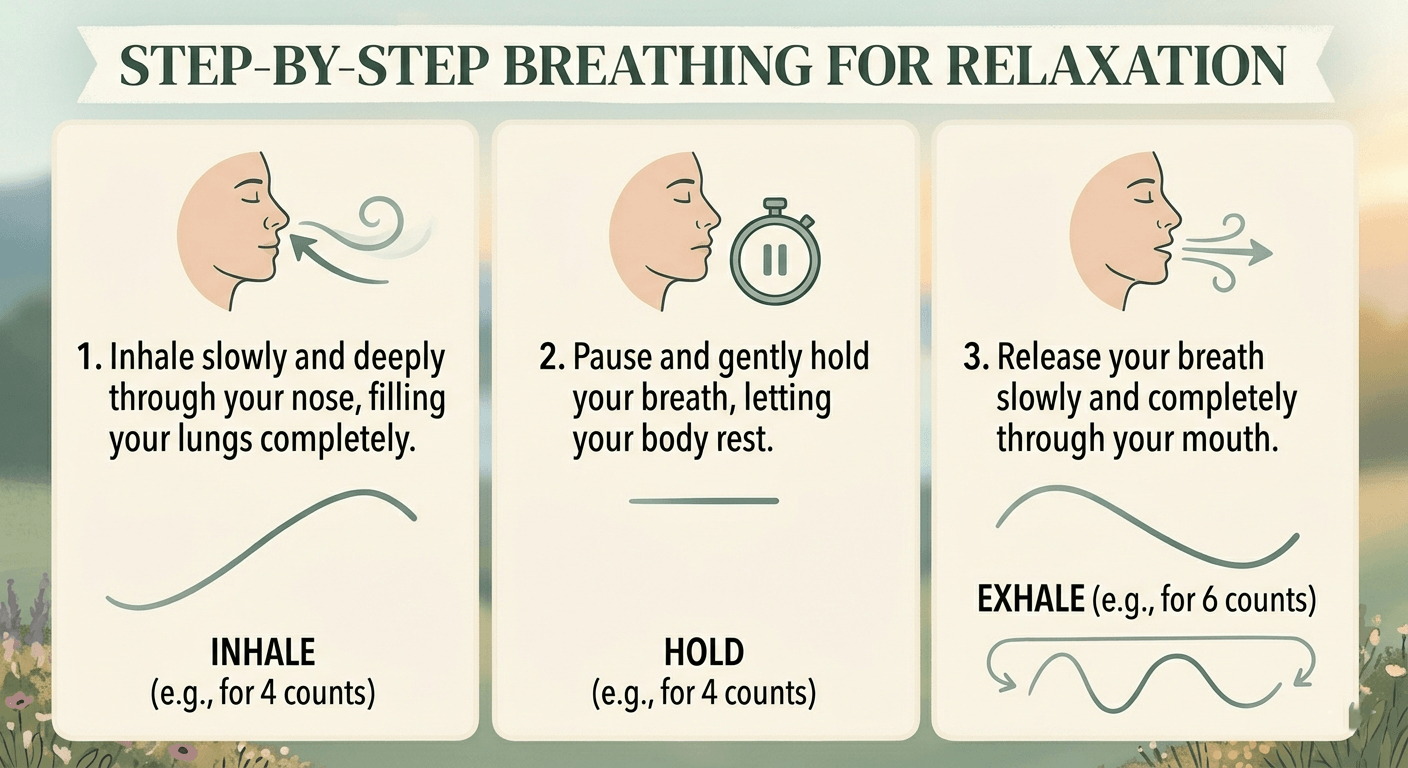
A Beginner’s Guide to Breathing Techniques
For those just starting out, it is wise to begin with low-intensity, regulating techniques that support the body’s natural “rest and digest” response.
Diaphragmatic “Belly” Breathing
The foundation of most breathwork is diaphragmatic breathing, which engages the large muscle at the base of the lungs.
- Technique: Sit or lie comfortably. Place one hand on your belly and the other on your chest.
- Action: Inhale slowly through your nose, allowing the belly and hand to rise while the chest stays relatively still. Picture a balloon gently expanding in your abdomen.
- Exhale: Breathe out through pursed lips as if softly blowing bubbles, feeling the belly fall.
- Benefit: This technique may help reduce cortisol and inflammation while sending signals of safety to the brain through the vagus nerve.
Box Breathing (The 4-4-4-4 Method)
Used by elite athletes and military personnel, box breathing is an excellent grounding tool under pressure.
- Protocol: Inhale for a count of 4, hold for 4, exhale for 4, and hold for 4.
- Mechanism: The even rhythm may help slow the heart rate and trains the mind to tolerate stillness.
- Visual Aid: Many find it helpful to picture tracing the four sides of a square with each part of the breath.
The 4-7-8 Relaxation Technique
Popularised by Dr. Andrew Weil, this method is sometimes called the “natural tranquiliser” for the nervous system.
- Steps: Inhale quietly through the nose for 4 counts, hold for 7 counts, then exhale audibly through the mouth for 8 counts.
- Focus: The extended exhale is the key component — it may stimulate the vagus nerve more powerfully than the inhale.
- Use Case: This is particularly well-suited to managing intrusive memories before sleep or de-escalating after a stressful encounter.
Alternate Nostril Breathing (Nadi Shodhana)
This ancient yogic practice is used to balance the left and right hemispheres of the brain and bring the autonomic nervous system into harmony.
- Action: Use the right thumb to close the right nostril and inhale through the left. Close the left nostril with the ring finger, release the thumb, and exhale through the right. Inhale through the right, close it, and exhale through the left.
- Outcome: Research suggests that regular practice may help support healthy blood pressure and heart rate levels while promoting a sense of well-being.
Advanced and Activating Breathwork Modalities
As beginners build confidence and nervous system capacity, they may choose to discover more “activating” approaches designed for deeper emotional release and catharsis.
Holotropic Breathwork and Non-Ordinary States
Developed by Stanislav Grof, Holotropic Breathwork (meaning “moving toward wholeness”) uses rapid, circular breathing and evocative music to bring about altered states of consciousness.
This approach is grounded in the idea that these states can awaken an “inner healer,” allowing the practitioner to process repressed memories stored in the limbic brain. Due to its intensity, it is traditionally practised in long sessions (up to 3 hours) with trained facilitators and “sitters” present for safety.
BioDynamic Breathwork & Trauma Release System (BBTRS)
BBTRS is specifically designed to address “somatic memory” — the understanding that trauma may be held in the body’s tissues.
- Six Elements: It combines breath with movement, sound, touch, emotional expression, and meditation.
- Process: Practitioners use “conscious connected breathing” — a continuous flow without pauses — to oxygenate the body and release suppressed emotions.
- Goal: Complete the biological survival responses (shaking, vocalising) that may have been interrupted during the original traumatic event.
The Wim Hof Method and Stress Inoculation
The Wim Hof Method combines specific breathing cycles (30–40 deep breaths followed by a breath hold) with cold exposure. From a trauma perspective, this functions as “stress inoculation” — by intentionally activating the sympathetic nervous system in a controlled environment, practitioners may build a higher tolerance for stress and a greater capacity to return to calm.
Managing Side Effects and Practising Safely
While breathwork can be a powerful healing tool, it is a physiological intervention that may produce strong physical and emotional reactions. Understanding what to expect helps keep the practice safe and supportive.
Physical Phenomena: Tetany and Hypocapnia
During intensive breathwork, the rapid release of carbon dioxide can lead to respiratory alkalosis, which may cause “tetany” — involuntary muscle contractions, typically in the hands, feet, or face. Sometimes referred to as “lobster claws,” these contractions are generally harmless but can feel uncomfortable or alarming.
Other common side effects include dizziness, tingling in the extremities (paresthesia), and sudden temperature shifts.
Emotional Catharsis
Breathwork is designed to move emotions through the body. It is not uncommon to experience intense emotional releases during sessions — crying, shaking, or vocalising are all within the normal range.
These are often deeply cathartic, but they need to be held within a safe, supportive container to support integration rather than further dysregulation.
The Risk of Re-traumatisation
The most significant risk in trauma-informed breathwork is re-traumatisation. For some people, the physical sensations of breathwork — such as chest tightness or a feeling of being “out of control” — can echo the sensations experienced during the original trauma.
If a facilitator is not trained to recognise the signs of a “false suffocation alarm” or a dorsal vagal shutdown, a session may inadvertently reinforce the trauma response rather than resolve it.
Breathwork Side Effects & Management
Understanding physiological responses and practical strategies for safe practice
| Side Effect | Physiological Cause | Management Strategy |
|---|---|---|
| Tetany | Hypocapnia / blood pH shift | Slow breathing; return to nasal breathing |
| Dizziness | Change in oxygen/CO₂ balance | Grounding; focus awareness on the feet |
| Flashbacks | Limbic brain activation | Resourcing, titration, pendulation |
| Panic Attack | Mimicking hyperventilation pattern | Transition to long exhales (4-7-8) |
Contraindications: Who Should Exercise Caution
Breathwork is generally safe, but certain conditions require medical supervision or specific modifications. Always consult your healthcare provider before starting breathwork if you have any of the following:
Breathwork Contraindications
Conditions requiring caution or medical supervision before practice
| Condition | Precaution |
|---|---|
| Pregnancy (especially 2nd/3rd trimester) | Avoid breath holds Consult your obstetrician before starting |
| Uncontrolled hypertension | Avoid rapid or forceful breathing Monitor blood pressure regularly |
| Epilepsy or seizure disorder | ⚠️ Hyperventilation may trigger seizures Only practice under medical supervision |
| Glaucoma | Breath holding increases intraocular pressure Avoid breath retention techniques |
| Recent abdominal or chest surgery | Consult surgeon before diaphragmatic work Wait for full clearance |
| Bipolar disorder with mania | Activating breathwork may trigger episodes Use only calming techniques |
| Severe asthma or COPD | Use caution Keep rescue inhaler nearby; avoid breath holds |
| Cardiovascular disease (arrhythmias, heart failure) | Avoid breath holds Consult cardiologist before starting |
| History of psychosis or schizophrenia | Only under psychiatric guidance Avoid intense or activating techniques |
| Severe PTSD with frequent dissociation | Start only with trained trauma-informed facilitator Never practice alone during early stages |
Related Questions and Specialised Topics
Making sense of the wider landscape of trauma recovery often leads beginners to related concepts — trauma bonds, inner child healing, and the role of holistic therapies, among them.
Healing from Emotional Abuse and Trauma Bonds
A “trauma bond” is a powerful emotional attachment to an abusive individual, often maintained by cycles of intermittent reinforcement. For survivors of emotional abuse, the nervous system can become conditioned to experience criticism and instability as “normal.”
The invisible aspects of trauma — including emotional and psychological harm that others cannot see — are often among the hardest to name and heal. Breathwork may be particularly valuable here, helping survivors reconnect with their own somatic cues. By building a safe internal state, breathwork can support the capacity to recognise warning signs and maintain boundaries without the emotional collapse that conflict might otherwise trigger.
Inner Child Healing through Somatic Awareness
Inner child work focuses on meeting the unmet needs and painful memories of the “child self” — the parts of us that were hurt or overlooked during development. Breathwork may support this process by creating the physiological steadiness needed for the nervous system to stop bracing, allowing reflective prompts to reach the inner child from a place of genuine safety.
Affirmations such as “You are safe now” or “You are loved” may be more deeply integrated when the body is in a parasympathetic state.
Complementary Holistic Approaches
Breathwork is frequently used alongside other therapeutic modalities:
- Ketamine Integration: Following ketamine therapy, breathwork may support neural rewiring and help consolidate insights into lasting behavioural shifts.
- Substance Recovery: For those managing withdrawal (for example, from tramadol or alcohol), slow-exhale breathing may help reduce panic and muscle tension. If you are also exploring gentle, body-informed approaches to detoxification, breathwork can be a calming complement to that process.
- Somatic Therapy: Modalities such as Somatic Experiencing (SE) or Sensorimotor Psychotherapy often draw on breathwork as a central tool for releasing tension held in the nervous system as a result of trauma.
Breathwork Training and Facilitator Accreditation
Because breathwork is currently an unregulated field, it is important for both practitioners and those training as facilitators to understand the value of accreditation and ethical standards.
Accrediting Bodies and Industry Standards
The Global Professional Breathwork Alliance (GPBA) is widely regarded as the benchmark for breathwork training accreditation. Schools accredited by the GPBA are required to follow a strict code of ethics, prioritise student safety, and provide thorough training in anatomy, physiology, and trauma-informed facilitation.
Other notable organisations include the International Breathwork Foundation (IBF) and the UK Breathwork Association (UKBA).
Key Components of High-Level Training
Professional programmes for those seeking to become trauma-informed facilitators typically include:
- Clock Hours: Rigorous programmes range from 50 to over 450 hours of study.
- Supervised Practice: Requirements often include facilitating a set number of documented sessions under a senior instructor.
- Nervous System Science: An in-depth look at Polyvagal Theory, respiratory physiology, and the mechanics of the vagus nerve.
- Professional Ethics: Guidance on boundaries, contraindications, and the professional scope of practice.
Looking Ahead in Somatic Trauma Resolution
Breathwork has moved well beyond the periphery of wellness to become a meaningful pillar of trauma-informed care. Its strength lies in its capacity to address the physiological roots of traumatic stress — offering a direct pathway to nervous system regulation that cognitive approaches may not always reach.
For beginners, the journey starts with simple, regulating practices like diaphragmatic breathing and box breathing, which build the capacity to safely work with more intensive modalities in time.
The somatic frameworks of resourcing, titration, and pendulation are not merely safety precautions — they are therapeutic necessities that help make healing sustainable and integrative.
As clinical research continues to bring ancient practices into the light of modern neuroscience, breathwork is well-positioned to become an increasingly accessible and vital tool for trauma survivors seeking to reclaim their lives from the imprints of the past.
Its deepest promise is the restoration of the social engagement system — a supported move from survival and isolation into connection, resilience, and a fuller sense of aliveness. If this guide has sparked your interest in transforming your mind and body naturally, breathwork is one of the most accessible and evidence-informed places to begin.
Breathwork for Trauma Healing
Frequently Asked Questions — Nervous System Recovery
Your health is in your hands.
Begin with your breath, and let us guide you towards a more balanced and empowered lifestyle.