Guide to Nervous System Regulation Techniques at Home in the United Kingdom

The Context of Nervous System Health in Great Britain
Your nervous system is the body's primary control centre — a remarkable network that manages everything from your heart rate and digestion to your emotional responses and ability to think clearly. Yet for many people across the United Kingdom, this vital system is quietly under siege.kenhub
When your body becomes locked in a chronicstressresponse, we call this a dysregulated nervous system . What makes it particularly challenging is that many people do not realise it is happening until the symptoms become impossible to ignore .ashfordstpeters.nhs
The numbers tell a sobering story. According to the Health and Safety Executive's 2024/25 figures, approximately 964,000 workers in Great Britain reported work-related stress, depression, or anxiety — a significant rise from 776,000 the previous year. This crisis hits hardest in the public sector, with central government, local government, health, and education all reporting the highest levels of concern
🌿 UK Workplace Health Metrics
| Workplace Health Metric | 2024/25 Statistical Value | Source / Reference |
|---|---|---|
| Workers with work-related ill health | 1.9 million | vinciworks |
| New cases of work-related ill health | 730,000 | hse.gov |
| Working days lost due to stress and anxiety | 22 million | hse.gov |
| Annual cost of work-related ill health to the UK | £22.9 billion | hse.gov |
| Estimated cost of mental ill health in England | £300 billion | vinciworks |
A dysregulated nervous system can show up differently for each person. You might notice constant worry, difficulty concentrating, or persistent poor sleep. On the physical side, frequent headaches, digestive problems, and chronic fatigue are common signals. When your system is out of balance, you tend to stay in a high-alert, survival-focused state — and this prevents your body from accessing its natural healing capacity .ashfordstpeters.nhs
Physiological Foundations of Regulation
The central nervous system — made up of your brain and spinal cord — works alongside your autonomic nervous system to manage how you respond to the world around you. These two branches of the autonomic nervous system need to work in harmony.kenhub
The Sympathetic Nervous System
This is your fight, flight, or freeze response. When your brain perceives a threat, the hypothalamus triggers a release of cortisol and adrenaline. Your heart rate rises and blood flow shifts toward your muscles. While this response is essential for survival in moments of genuine danger, keeping it switched on long-term takes a serious toll — including sustained strain on your heart and arteries.byjus
The Parasympathetic Nervous System
This branch does the opposite: it promotes rest, recovery, and what is often called the "rest and digest" state. The vagus nerve is its most significant component, running from your brain to your internal organs. Activating this nerve is a central goal of most regulation techniques, as it sends a clear signal to your brain that you are safe.mind.org
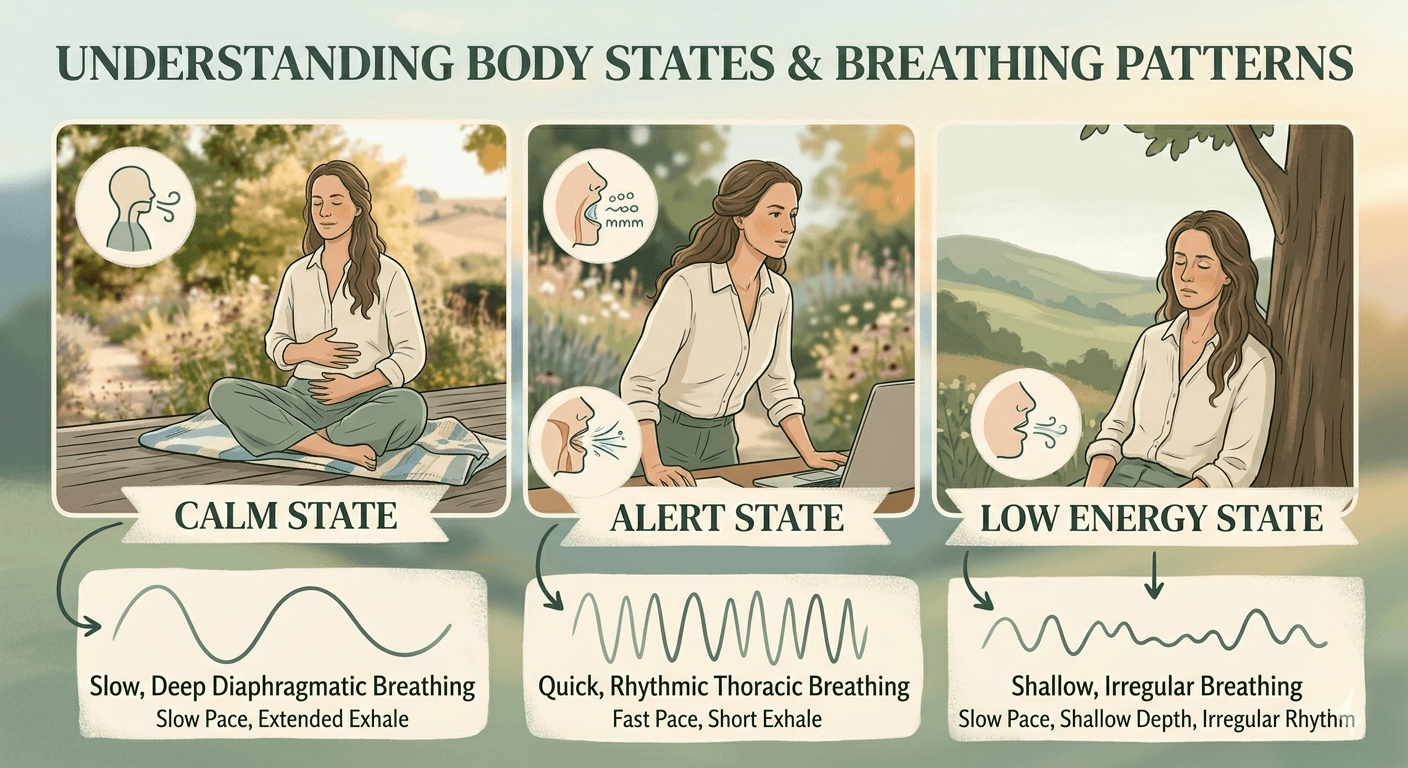
The interplay between these two systems determines what therapists call your window of tolerance — the zone in which you can handle stressors without becoming overwhelmed. Stay within this window and you feel grounded and present. If a stressor exceeds what you can manage, you may tip into hyperarousal (agitation, panic, a racing heart) or hypoarousal (numbness, disconnection, fatigue).polyvagalinstitute
Nervous System States
| Nervous System State | Common Sensations and Behaviours | Polyvagal Reference |
|---|---|---|
| Ventral Vagal (Safety) | Grounded
Curious
Connected
Calm
Social engagement
Present-focused
|
polyvagalinstitute |
| Sympathetic (Activation) | Anxious
Irritable
Racing heart
Focused / hyperalert
Restless
Rapid thoughts
|
polyvagalinstitute |
| Sympathetic (Dysregulation) | Overwhelmed
Angry / rageful
Shallow breathing
Panic
Hypervigilance
Unable to settle
|
polyvagalinstitute |
| Dorsal Vagal (Shutdown) | Numb
Disconnected
Hopeless
Fatigued / exhaustion
Dissociation
Collapse
|
polyvagalinstitute |
Breathing Protocols for Home Practice
Breathing occupies a unique place in the regulation toolkit — it is the only physiological function that operates both automatically and under conscious control. This makes it an incredibly effective bridge between mind and body. Deep, intentional breathing stimulates the vagus nerve and helps to lower cortisol levels.nhs
Diaphragmatic Breathing Technique
Many of us in the UK breathe using only the upper part of our chest — a pattern that tends to become more restricted during periods of anxiety . This shallow breathing does not draw on the full capacity of the lungs .nhs
To practise diaphragmatic breathing, sit or lie in a comfortable position and place one hand on your chest and the other on your abdomen . Breathe in slowly through your nose for four seconds. Your abdomen should rise while your chest stays relatively still . Hold for two seconds, then exhale fully through your mouth, watching your abdomen move inward . Aim for at least five minutes of this each day .nhs
The Box Breathing Method
This highly structured technique is particularly useful during moments of acute stress and has been shown to improve heart rate variability.bhf.org
Inhale through your nose for a count of four.
Hold for a count of four.
Exhale through your mouth for a count of four.
Hold again for a count of four.
Repeat for several minutes until you feel a shift.bhf.org
The 4-7-8 Relaxation Exercise
This method can calm an overactive nervous system remarkably quickly and is especially useful for those who struggle with sleep. Place the tip of your tongue against the ridge of tissue just behind your upper front teeth. Exhale completely through your mouth with a "whoosh" sound. Inhale quietly through your nose to a count of four. Hold for a count of seven. Exhale through your mouth for a count of eight. Repeat for four full cycles. The extended exhale is the most powerful part — it actively signals safety to your brain.bhf.org
The Physiological Sigh
This is one of the fastest ways to ease anxiety in real time . Take a deep breath in through your nose, and at the very top of that breath, take a second, shorter sip of air to fill your lungs completely . Then exhale slowly and fully through your mouth . Two or three repetitions can reset your system within seconds .stgeorges.nhs
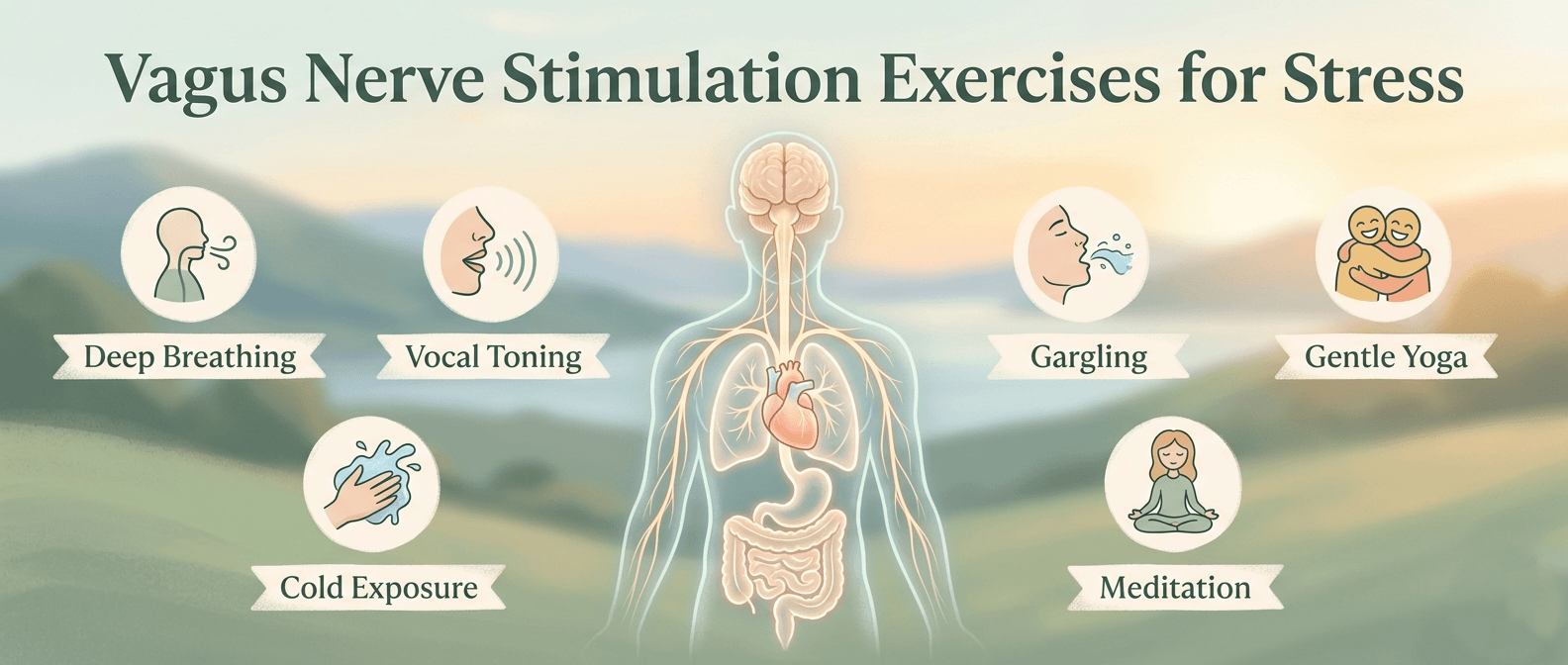
Vagus Nerve Stimulation at Home
Your vagus nerve plays a fundamental role in your parasympathetic response. There are several straightforward ways to stimulate it using nothing more than your own body and everyday household items.mind.org
Vocal Exercises
The vagus nerve connects directly to your vocal cords, meaning mechanical vibrations in your throat can activate it.
Humming a familiar tune is a gentle starting point — pay attention to the sensations in your head and chest as you do it. Research suggests that five minutes of humming can measurably reduce stress scores. Singing loudly, chanting, or sounding out a long "voo" on an extended exhale are equally effective. This vibration sends a safety signal directly to your brainstem.mind.org
Gargling with water is another surprisingly potent method. Gargle vigorously — to the point where you almost gag — to activate the branches of the vagus nerve that run through the back of your throat.mind.org
Auricular Massage
Specific points on your outer ear sit closest to the surface of the vagus nerve, making ear massage a discreet and accessible technique .stgeorges.nhs
Try the cymba swizzle: place the tip of your finger in the hollow of your outer ear just above the earlobe and massage gently in a circular motion . You may find yourself yawning — a reliable sign that your parasympathetic nervous system is becoming active . Ear tugging is another option: gently pinch your earlobe and pull it downward, then work your way up the outer rim. You are aiming to trigger a nerve response that may produce a sigh — nature's own reset
button.mind.org
Thermal Regulation and Cold Exposure
Cold water exposure is a remarkably fast way to recalibrate your system. It triggers the mammalian diving reflex, which slows the heart rate and redirects blood flow toward the brain .stgeorges.nhs
At home, you can splash ice-cold water on your face for around fifteen seconds. Holding an ice pack or a bag of frozen peas against the side of your neck works well too, as does placing a cold, damp cloth at the back of your neck. If you are feeling more adventurous, finishing your shower with thirty to sixty seconds of cold water builds long-term stress resilience over time.stgeorges.nhs
Cold Exposure Methods
| Cold Exposure Method | Recommended Duration | Physiological Goal |
|---|---|---|
| Face splashing | 15 seconds | Trigger diving reflex |
| Ice pack to neck | 30 seconds | Vagus nerve stimulation |
| Ice cube holding | 1 minute | Sensory grounding |
| Cold shower finish | 30–60 seconds | Build hormetic resilience |
Please speak to your GP before starting intense cold exposure if you have a heart condition or any cardiovascular concerns
Somatic Movement and Grounding Techniques
Stress does not just live in the mind — it accumulates as physical tension in your muscles and connective tissue. Somatic movement techniques work by helping to discharge this stored energy and return the body to balance.
The Shaking Practice
Animals instinctively shake after a frightening experience to release survival energy from their bodies. Humans can do this too. Stand with your feet hip-width apart and begin by lightly shaking your hands and wrists, letting the movement spread up through your arms and shoulders. Bounce gently on your heels to send a rhythmic vibration through your whole body. Keep this going for two to five minutes — it is a surprisingly effective way to release built-up tension from your fascia and muscles.nhs
Progressive Muscle Relaxation (PMR)
This technique teaches your brain to recognise the difference between physical tension and ease by deliberately moving through both states. Lie down comfortably and start with your toes. Curl them tightly for five seconds, then release completely and notice the change. Move to your calves, then your thighs, abdomen, hands, and finally your face. Finish by scrunching all your facial muscles at once, then letting your whole body go limp. The contrast can be deeply settling.nhs
Sensory Grounding Protocols
Grounding techniques help you stay present when anxiety pulls your thoughts into a spiral. The 5-4-3-2-1 technique is one of the most widely used: name five things you can see, four things you can feel (like the texture of your clothing), three things you can hear, two things you can smell, and one thing you can taste.nhs
You can also try a "palm buddy" — a small object with a distinct texture, such as a smooth stone or a fidget toy . Focusing on its weight and surface helps anchor you to the present moment . Simply noticing the contact between your feet and the floor can be equally grounding,stgeorges.nhs
Floor-Based Regulation
Lying flat on your back on a rug or yoga mat gives your brain clear information about where you are in space. This firm, stable contact helps your nervous system feel safe and organised. Making slow, wide arm movements — similar to snow angels — while lying down encourages both sides of the brain to work together, producing a calming, integrating effect. Think of it as a natural reset after a high-energy period.
Holistic Lifestyle and Nutritional Support
Regulation is not just about managing moments of crisis. It is about building a strong foundation through your everyday habits and choices.
Nutrition for Nerve Health
Your nervous system depends on a steady supply of energy and specific nutrients to function well. Skipping meals or relying heavily on sugar can make dysregulation worse by causing energy crashes that trigger a stress response.
Certain foods offer real support. Turmeric contains curcumin, which has anti-inflammatory effects on the nervous system. Oily fish like salmon provides omega-3 fatty acids that support brain function and help to reduce anxiety. Dark chocolate contains flavonols that increase blood flow to the brain.
Essential Nutrients
| Essential Nutrient | Role in Regulation | Top UK Food Sources |
|---|---|---|
| Omega-3 (DHA/EPA) | Maintenance of brain function | Salmon
Mackerel
Algae
|
| Magnesium | Supports 300+ biochemical processes | Pumpkin seeds
Leafy greens
|
| Vitamin C | Supports nervous system function | Goji berries
Citrus fruits
|
| Iodine | Normal nervous system operation | Prunes
Seaweed
|
| B-Vitamins | Energy production and mood | Whole grains
Eggs
|
The MIND diet — which combines principles from the Mediterranean and DASH diets — offers a practical framework for supporting nerve health. It focuses on plant-based foods, nuts, and berries. Research consistently shows that a plant-rich diet benefits gut health, and your gut plays a significant role in mood through its production of neurotransmitters like serotonin.
Herbal Remedies
Many traditional herbs have long been used in the UK to support a balanced nervous system. Valerian root is often recommended for sleep difficulties, as it works by reducing the breakdown of GABA in the brain — a process that helps regulate nerve impulses and promote calm. Chamomile, lemon balm, and passionflower are widely valued for their calming, anti-anxiety properties.
Always speak to your GP before beginning new herbal supplements, particularly if you take prescribed medications.
The Role of Sleep Hygiene
Sleep is when your brain does much of its emotional processing. During deep REM sleep, your brain works through the experiences of the day. Without this nightly restoration, you are far more likely to feel reactive, irritable, and emotionally raw.
To improve sleep quality, set a consistent bedtime and wake time and stick to it. Avoid screens for at least an hour before bed — the blue light they emit interferes with melatonin production. The NHS notes that reduced light exposure at certain times of year can further disrupt your body's natural rhythms, making consistent sleep hygiene especially important during winter months (NHS, n.d.b). Keeping your bedroom cool, dark, and quiet sends clear signals to your body that it is time to rest.
Managing the UK Winter Season
Winter in the United Kingdom brings its own challenges for the nervous system. Reduced daylight hours can affect your circadian rhythm and lower serotonin levels. The NHS recognises that this seasonal shift contributes to low mood for a significant proportion of the UK population (NHS, n.d.b).
Biological Sensitivity to Cold
Cold temperatures physically slow down nerve conduction, meaning electrical signals travel more slowly through your body. You might notice morning muscle stiffness or a general sense of sluggishness. For those living with conditions like Multiple Sclerosis or Parkinson's, winter can intensify symptoms noticeably.
Cold weather also causes blood vessels to constrict — a process called vasoconstriction — which reduces blood supply to the nerves and can increase sensations of pain or numbness in the limbs.
Strategies for Seasonal Resilience
Getting outside during the brightest part of the day is one of the simplest and most effective things you can do. Even ten minutes of natural light exposure helps to set your internal body clock (NHS, n.d.b). Warming foods — soups and stews made with whole ingredients — support stable blood sugar and sustained energy. Staying hydrated is also important, since cold weather blunts your awareness of thirst. And do not underestimate the power of genuine human connection: face-to-face time with others releases oxytocin, which actively counters stress hormones.
Winter Wellbeing Strategy
| Winter Wellbeing Strategy | Practical Action | Benefit for Nervous System |
|---|---|---|
| Maximise Daylight | Use a SAD lamp or walk at noon | Stabilises serotonin and melatonin |
| Thermal Comfort | Use weighted blankets and layers | Provides calming deep pressure |
| Consistent Rhythm | Wake up at the same time daily | Supports circadian health |
| Mindful Movement | Home yoga or indoor stretching | Reverses cold-induced stiffness |
Workplace Stress and Employer Standards
For many people in the UK, the workplace is the primary source of nervous system stress . Managing how you respond at work is essential for long-term health.
Strategies for the Professional Environment
Subtle regulation techniques can make a real difference throughout the working day. Taking a short break every 90 minutes — even just standing up and stretching, or doing two minutes of box breathing — helps prevent the stress accumulation that builds when we sit and push through for hours.
If you feel overwhelmed during a meeting, try a brief orienting practice: notice the colours and shapes in the room without judging them. Check your posture — if you are slumping, lengthening your spine can send a signal of alertness and safety to your brain. And if adrenaline is making you anxious, consider redirecting that energy toward a task that genuinely needs your focus.
The Responsibility of UK Employers
UK employers have a legal duty to protect the mental health of their workers, as far as is reasonably practicable . The Health and Safety Executive is actively scrutinising organisations for failures in managing mental health risks (Health and Safety Executive, 2025b). A genuinely supportive workplace culture makes co-regulation possible — this happens when leaders model calm behaviour and practise empathetic listening. Regular risk assessments for stress, staff training to recognise signs of dysregulation, and addressing root causes like excessive workloads are all essential components of a healthy workforce (Health and Safety Executive, 2025a).
Advanced Regulation Options and UK Research
Home techniques are highly effective for daily maintenance, but some people will benefit from professional support for deeper or more persistent dysregulation.
UK Clinical Trials and Innovation
The UK is actively contributing to research into nervous system regulation. The University of Nottingham and the University of Cambridge are collaborating on studies using ultrasound to stimulate the vagus nerve — a method that may prove more targeted than electrical stimulation (National Institute for Health and Care Research, n.d.). The University of Leeds is running a pilot study on non-invasive vagus nerve stimulation (nVNS) for chronic musculoskeletal pain (ClinicalTrials.gov, n.d.). A study at University College London found that 30 minutes of daily vagus nerve stimulation improved fitness levels, increased oxygen uptake, and reduced inflammation in participants — pointing to real potential for people living with heart failure (University College London, 2025).
UK University Research Sites
| UK University Research Site | Focus Area / Technology |
|---|---|
| University of Leeds | Chronic MSK Pain — gammaCore Sapphire (nVNS) |
| UCL / Queen Mary | Exercise Tolerance — Auricular Ear Clip Stimulator |
| University of Liverpool | Epilepsy (VNS-ALERT) — Implanted VNS device |
| University of Glasgow | Stroke Recovery — VNS paired with Physiotherapy |
| University of Nottingham | Anxiety and Depression — ZenBud Ultrasound |
Professional Therapeutic Pathways
If you consistently feel stuck in survival mode, speaking with your GP is an important first step. The NHS provides several mental health support pathways. NHS Talking Therapies remains the backbone of provision in England, offering Cognitive Behavioural Therapy (CBT) to help identify and shift negative thought patterns . Eye Movement Desensitisation and Reprocessing (EMDR) is an evidence-based treatment recommended by NICE for PTSD.
Somatic therapies focus on the body-mind connection, helping you reconnect with bodily sensations and release stored energy from past trauma. Some practitioners use the Safe and Sound Protocol (SSP) — a technique that uses specially filtered music to help retune the nervous system toward a state of safety.
Building a Sustainable Daily Toolkit
Consistency is the most important ingredient in changing your nervous system over time. Small, regular practices build real resilience in a way that occasional effort simply cannot.
Morning Momentum
Start your day with five minutes of intentional breathing to set a calm baseline. If you can, spend time in a green space — research shows that even twenty minutes in nature can significantly reduce cortisol levels.
Midday Pause
Check in with yourself throughout the day. Ask yourself whether you are within your window of tolerance. If you notice tension rising, try the neck stroke: gently run your fingers down the ridge of muscle connecting your ear to your collarbone. It often triggers a yawn and gently signals your body to ease up.
Evening Wind-Down
Create a screen-free routine at the start of your evening. Gentle stretching, restorative yoga, or therapeutic journaling all support the transition into rest. Writing your thoughts down creates a helpful distance between a stressor and your reaction.
A gratitude practice is worth adding to - research suggests that recording things you are grateful for regularly can meaningfully shift your outlook within ten weeks.
Daily Rituals
| Daily Ritual | Specific Technique / Goal |
|---|---|
| Morning | 5 minutes of Box Breathing — set physiological baseline |
| Midday | 20-minute park walk — reduce cortisol levels |
| Afternoon | 10-minute gentle yoga — release physical tension |
| Evening | Screen-free wind-down — support melatonin production |
Frequently Asked Questions
Your nervous system is an elaborate communication network that shapes your entire experience of life. Modern life in the UK places intense demands on this system, often leading to chronic stress and declining health . But through breathing exercises, somatic movement, and thoughtful lifestyle changes, reclaiming your calm and building genuine resilience is within reach .
Every small habit you build helps to rewire your nervous system toward balance. At its heart, regulation is about flexibility — the ability to meet life's challenges and then return to a place of peace and recovery. That foundation is what makes a truly balanced and fulfilling life possible.
References
Ashford & St Peter's Hospitals NHS Foundation Trust. (n.d.). Nervous system regulation. https://www.asph.nhs.uk/nervous-system-regulation
ClinicalTrials.gov. (n.d.). Non-invasive vagus nerve stimulation for chronic musculoskeletal pain (Study NCT07409363). U.S. National Library of Medicine. https://clinicaltrials.gov/study/NCT07409363
Health and Safety Executive. (2025a). Key figures for Great Britain 2024 to 2025. https://www.hse.gov.uk/statistics/overview.htm
Health and Safety Executive. (2025b). HSE publishes annual workplace health and safety statistics Press release. https://press.hse.gov.uk/2025/11/20/hse-publishes-annual-workplace-health-and-safety-statistics/
National Institute for Health and Care Research. (n.d.). Non-invasive ultrasonic auricular vagus nerve stimulation (Trial ID: 59400). Be Part of Research. https://bepartofresearch.nihr.ac.uk/trial-details/trial-detail?trialId=59400
NHS. (n.d.a). Breathing exercises for stress. https://www.nhs.uk/mental-health/self-help/guides-tools-and-activities/breathing-exercises-for-stress/
NHS. (n.d.b). Seasonal affective disorder (SAD). https://www.nhs.uk/mental-health/conditions/seasonal-affective-disorder-sad/
South West London and St George's Mental Health NHS Trust. (2024). World Mental Health Day 2024: Nervous system hacks for wellbeing. https://swlstg.nhs.uk/latest-news/world-mental-health-day-2024-nervous-system-hacks-for-workplace-wellbeing-2252
University College London. (2025, July). Vagus nerve stimulation could help people get more exercise. UCL News. https://www.ucl.ac.uk/news/2025/jul/vagus-nerve-stimulation-could-help-people-get-more-exercise